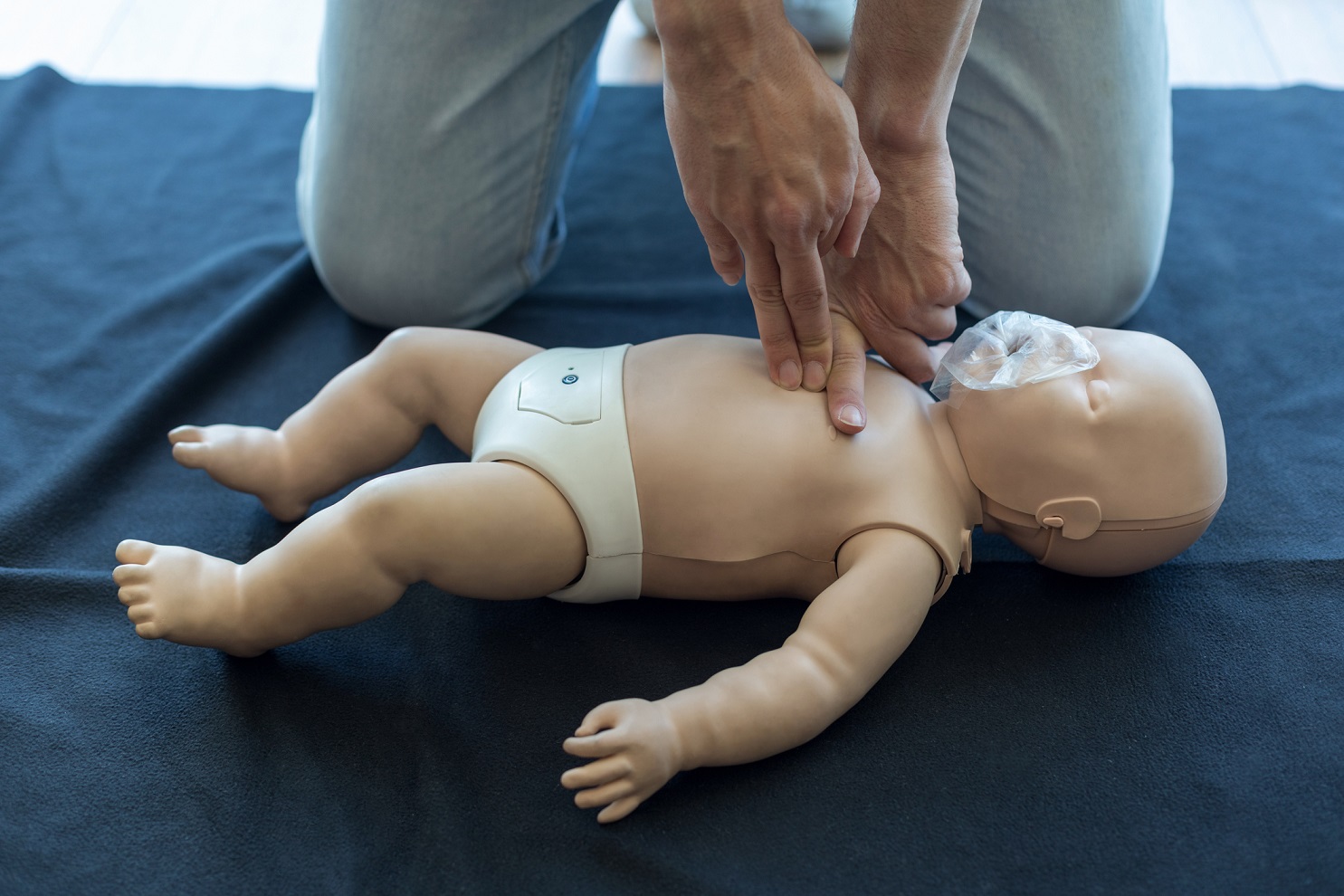
No one is too small for great care.
From primary care to specialty care and for everything in between, we are here to provide excellent care for children.
Excellent care begins with an excellent staff — from the surgeons who perform heart transplants, to the patient access specialists who greet patients, to the housekeeping assistants who keep our patients’ rooms clean and sanitary. One of the methods to ensure excellence from our staff is healthcare simulation.
Healthcare simulation is a range of activities used to provide real-world experiences in a manufactured environment, in order to improve safety, efficacy, and efficiency of healthcare services.
During a simulation, learners are trained to provide healthcare for different types of patients under a variety of circumstances — all without using live patients or jeopardizing safety.
Our most recent scenarios include:
- Housewide nursing reviews
- Crash cart races
- Team training
- Treatment of patient being transported by helicopter
- Transport of patient during airline fire
Set Up Your Simulation Training
Email [email protected]
Children’s Simulation Resources Provide You with the Best Educational Tools, Techniques & Resources
We invite all Children’s clinicians to take advantage of simulation services to help you provide the best care for your patients.
Our high fidelity simulation program uses a computer-driven, full-bodied simulators with physiological responses programmed to immediately “react” to your interventions. We have simulation tools available for developing many types of skills, including:
- General routine and emergency infant and neonatal care
- Advanced pediatric trauma surgery
- Specialty procedures, such as gastrostomy tube or urethral catheter insertion
- Medical devices for children with special needs
The Simulation Process
The Children’s Simulation process includes four phases:
Phase I: Empowering
We help empower you to develop and deliver simulations that are best suited for your learners’ needs. This phase involves defining the educational needs, learning objectives, and the tools needed to achieve the objectives.
Phase II: Engaging
By being engaged in creating the simulation, you are in control of what participants to experience and learn. This phase involves programming, reviewing, and editing the simulation, performing a dry run, and completing the set-up.
Phase III: Educating
The Educating Phase has two parts:
Simulation
This is when we actually run the simulation. In addition to learners and educators, the simulation room typically includes:
- A mannequin, on which can have procedures like intubation or CPR can be performed
- A patient monitor telemetry screen that shows the “patient’s” vital signs
- A simulation educator who uses a laptop to run the mannequin
- Emergency equipment, such as a code cart
- Lab and imaging equipment
Debriefing
The second part of Phase III is debriefing. This is the most important component of simulation, and where most of the learning actually takes place.
A facilitator leads a reflective discussion on the simulation. Learners can provide feedback on their performance, each other’s performance, reflect on team dynamics, communications or personal feelings during the simulation, and discuss how to apply the simulation experience in future situations.
Phase IV: Excelling
The final phase is outlining what you and your learners need to build on successes and learn from missteps. This involves getting learners’ evaluation of the simulation and debriefing, your analysis of the experience, and your feedback to improve the experience in the future.
Giving feedback to improve the simulation experience. After each simulation experience, please give us feedback by completing a brief survey.
+Zone of Proximal Development
Scenarios are designed according to the Zone of Proximal Development theory. That means we try to make scenarios just difficult enough to keep learners optimally engaged. If the scenario is too easy or too difficult, learners may become disinterested and disengaged, which undermines the educational experience.
Meet Our Team

Kelly D. Kadlec, MD
Simulation Medical Director
-
About Dr. Kadlec
Pediatric Intensivist
Children’s Nebraska – OmahaAssociate Professor, Pediatrics,
University Of Nebraska College of Medicine

Jessie Henry MSN, RN, CPN
Simulation Program Supervisor and Educator
-
About Jessie Henry MSN, RN, CPN
Jessie started her nursing career in 2013, spending some time working with the adult population prior to transitioning to the Pediatric Intensive Care Unit (PICU) at Nebraska Medicine in 2014. She joined the PICU team at Children’s Hospital and Medical Center in 2017, where she continued her work at the bedside. She has had the opportunity to care for many medically fragile, complex, and critically ill children in specialized areas including trauma, transplant, cardiology, and neurosurgery.Working in the critical care environment has allowed her to mature as a nurse, as a leader, and as an educator. In 2020, Jessie joined the simulation team part-time as a Simulation Educator with the intent to share her knowledge and experiences to help others grow and challenge themselves, while still having fun and learning. In 2021, Jessie graduated with her master’s degree in nursing education and officially transitioned to the Clinical Education department full time in the summer of 2022, taking on the role of the Simulation Program Supervisor. She is excited for the opportunity to teach others how to utilize their skills, respond in challenging situations, and further develop their critical thinking to prepare for unanticipated events.

Jamie Bussen BSN, RN, CPN
Simulation Educator
-
About Jamie Bussen BSN, RN, CPN
Jamie began her nursing career in 2007, working as a new graduate in the Pediatric Intensive Care Unit (PICU) at Children’s Nebraska. While working at the bedside, she increased her knowledge and skills. She discovered she had a passion for the ICU. She continued to work bedside in PICU, NICU, and CICU as a FLEX nurse until September 2022. In 2020, Jamie joined the Clinical Education Team as a Resuscitation Program Coordinator while continuing her work at the bedside. As a resuscitation Program Coordinator, she has taught many PALS and PEARS classes, analyzed data, worked on performance improvement projects and mentored other peers on the floor. She has an energetic personality that keeps all students engaged. In September 2022, Jamie joined the Simulation Education Team in a part time Simulation Educator Position. The combined roles of Resuscitation Program Coordinator and Simulation Educator gives her a unique advantage to educate peers and improve patient outcomes. She is excited to share her knowledge, experience, and energy to teach simulations. Jamie hopes to improve patient outcomes by educating others to help them be comfortable in emergency situations.

Charlotte Stuhr RN, BSN, CCRN
Simulation Educator
-
About Charlotte Stuhr RN, BSN, CCRN
Charlotte began her nursing career in 1997 at Ambassador Pediatrics then transferred to the PICU at UNMC. Charlotte realized that pediatric critical care was her passion yet wanted to incorporate a cardiac component to her knowledge base.In 2000 Charlotte moved to the PICU at Children’s Hospital where they had a combined PICU/CVICU. There she discovered her talent for teaching and precepting. She has served as PALS instructor, preceptor, nurse resident and transition to pediatrics instructor, and lectured in the Heart Smart series for the Cardiac Care Unit.
Charlotte utilizes her passion for pediatric critical care to help others develop the fundamentals of pediatric resuscitation. She places an emphasis on early recognition and anticipation. She wants people to learn to anticipate what might happen next and be at least two steps ahead of the patient. Her goal is to always make people feel comfortable and confident when learning how to take care of children in emergency situations.

Luke Palacio NRP, BS EMS
Simulation Educator
-
About Luke Palacio NRP, BS EMS
Luke began his career in healthcare in 2010, joining his local volunteer fire department as an EMT. He obtained his BS in Emergency Medicine, along with his paramedic license, from Creighton University in 2014, allowing him to pursue a permanent position within several emergency departments and Level 1 Trauma Centers throughout the Omaha area. During this time, he was able to utilize his experience and share his knowledge as an instructor for Creighton’s paramedic/EMT program.In 2018, Luke joined Children’s Hospital and Medical Center as one of the first inpatient paramedics in the Pediatric Intensive Care Unit (PICU). In his role at the bedside, Luke applied his critical thinking, unique skill set, and extensive experience to educate his peers, which led him to join the simulation program as a Simulation Educator in 2022. Luke enjoys utilizing high-fidelity simulation to assist others in further developing their knowledge, critical thinking skills, and confidence when caring for children during emergent situations.